Research & Evidence
Our commitment to evidence-informed, individualized pediatric care
At B.well tots, we believe families deserve to understand the “why” behind what we do.
Our approach integrates:
Current research
Clinical expertise
Ongoing professional training
Your child’s unique needs and responses
Below is a curated research bank organized by modality.
Low-Level Laser Therapy (LLLT) / Photobiomodulation for Infants & Children
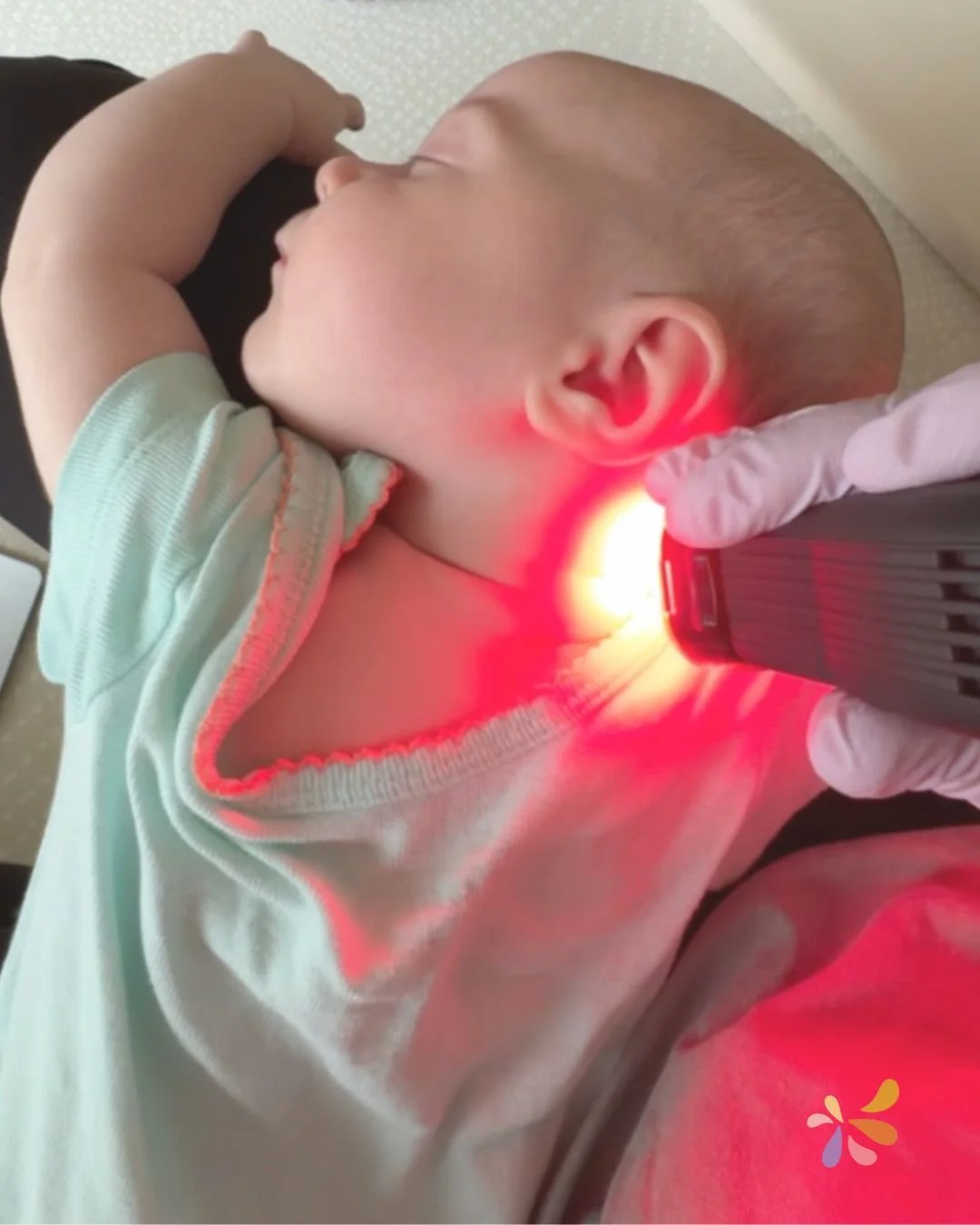
Low-Level Laser Therapy (LLLT), also known as photobiomodulation (PBM), has been investigated in various studies for its potential therapeutic effects in children.
It is a gentle, non-invasive therapy that uses low-intensity light to stimulate healing and improve cellular function.
Research shows that LLLT may help with:
Infant frenectomy (tongue-tie release) – reducing pain, swelling, and improving feeding outcomes
Speech and feeding – supporting swallowing, voice, and oral motor recovery
Neurodevelopment – enhancing emotional regulation, sleep, attention, and learning
Motor coordination and control – reducing spasticity, supporting muscle recovery, and improving motor function
Pain and inflammation – aiding recovery in oral, dental, and musculoskeletal conditions
Below is a comprehensive list of studies examining LLLT across pediatric populations, along with summaries and links for deeper reading.
Infant Frenectomy (Tongue-Tie Release) Research
LLLT is increasingly applied before and after frenectomy to support comfort, healing, and oral function.
LLLT in Pediatric Oral Surgeries
Reduces postoperative pain, swelling, and speeds up oral wound healing.
👉 PubMedPhotobiomodulation for Oral Wound Healing
World Association for Photobiomodulation Therapy (WALT) guidelines support PBM for pediatric oral wound care and pain relief.
👉 WALT GuidelinesInfant Frenectomy Case Reports
Reports show improved breastfeeding outcomes (better latch, less nipple pain) and faster recovery when PBM is used post-frenectomy.
👉 PubMed Case SummaryPBM in Oral Mucositis (Children with Cancer)
Demonstrates PBM’s ability to reduce oral pain and inflammation and promote mucosal healing—mechanisms directly applicable to frenectomy.
👉 Archives of Disease in ChildhoodLLLT for Pre-Anesthetic Tissue Management
PBM reduces tissue pain/tension in children before injections, suggesting benefit for pre-frenectomy preparation.
👉 BMC Oral HealthPBM in Feeding & Speech Rehabilitation
Studies in dysphagia and speech therapy show PBM supports swallowing, oral motor recovery, and functional feeding skills.
👉 SpringerLink – Dysphagia Study
Emotional Regulation, Sleep & Neurodevelopment
Research suggests that PBM may play a role in brain function and emotional well-being in children.
Transcranial PBM in Autism (Ages 2–6)
Randomized sham-controlled trial showed improvements in emotional regulation, attention, and behavioral symptoms.
👉 FrontiersPBM in Autism Spectrum Disorder
Studies report reduced irritability, emotional dysregulation, and behavioral challenges in children with ASD.
👉 ResearchGateNeuroplasticity & Cognitive Recovery
PBM enhances neuroplasticity, supporting recovery of speech, language, and cognitive functions in neurological conditions.
👉 PubMedSleep & Regulation
LLLT was used to reduce inflammation of tonsils to increase airway capacity and allow for improved sleep quality and decreased sleep disordered breathing with good success.
Motor Coordination & Control
LLLT has been studied for its effects on spasticity, strength, and muscle recovery in children.
Impact on Spasticity in Cerebral Palsy
Systematic review shows LLLT may reduce spasticity and improve motor outcomes.
👉 MDPILLLT in Cerebral Palsy (Motor Function)
Combined with functional training, LLLT improved gross motor outcomes in children.
👉 Neuro AcupuncturePBM + Physiotherapy in Myelomeningocele
Clinical trial showed improved functional performance and motor skills.
👉 MDPIEffect on Quadriceps and Foot Muscles
LLLT reduced muscle fatigue, improved strength, and supported exercise recovery in children.
👉 PubMed Central
Additional Pediatric Research
Children with Energy-Protein Malnutrition (1–5 yrs)
LLLT improved salivary biomarkers in malnourished children.
👉 PubMedLLLT in Cancer Therapy-Induced Oral Mucositis
Systematic review/meta-analysis confirmed LLLT reduces severity and pain.
👉 PubMedLLLT for Oral Mucositis in Cancer Patients
Demonstrated significant pain relief and faster recovery.
👉 SpringerLinkEffect on Condylar Growth (Mandibular Deficiency)
Enhanced condylar growth when paired with functional appliances.
👉 SpringerLinkOrthokeratology & LLLT for Myopia
Both treatments slowed myopia progression.
👉 Wiley Online LibraryPBM in Chemotherapy-Induced Oral Mucositis (AML)
Reduced incidence/severity of mucositis in pediatric leukemia patients.
👉 PubMedPBM Retarding Axial Length Growth in Myopia
PBM slightly slowed axial length growth in myopic children.
👉 NaturePBM for Injection Pain in Children
Reduced pain perception during injections.
👉 BMCCurcumin vs PBM in Oral Mucositis
Both improved outcomes in cancer-related mucositis management.
👉 SpringerLink
Speech Therapy Applications of LLLT
LLLT is increasingly relevant to speech-language pathology (SLP).
Voice Disorders – Reduced inflammation, improved voice quality.
👉 PubMedAphasia Recovery – PBM promotes neuroplasticity and aids language recovery.
👉 PubMedTMJ Disorders – Reduced pain, inflammation, improved function.
👉 PubMedClinical Overview in SLP – Safe integration into therapy for voice, dysphagia, and aphasia.
👉 PubMedSwallowing Rehab – Reduced pain and inflammation in swallowing muscles.
👉 PubMedInflammatory Cytokines & TMJ Pain – LLLT lowered cytokines and pain.
👉 PubMedNeurological Speech Disorders – Improved motor control in dysarthria and apraxia.
👉 PMC
Key Takeaways
LLLT/Photobiomodulation is a safe, evidence-backed therapy with wide applications in pediatric care:
Frenectomy support – Faster healing, less pain, improved feeding
Speech/feeding therapy – Supports swallowing, voice, and oral motor recovery
Neurodevelopment – Enhances regulation, attention, and sleep
Motor rehabilitation – Improves muscle performance and coordination
Pain & inflammation – Gentle relief across oral, dental, and musculoskeletal needs
🔴 Low-Level Laser Therapy (LLLT) / Photobiomodulation
Evidence Level: Strong (Medical) + Emerging in Pediatrics
LLLT is well-supported in medical and dental research for healing, inflammation, and pain modulation.
Key Research:
Pediatric photobiomodulation in dentistry (review)
https://europepmc.org/article/MED/31873064LLLT for oral mucositis in pediatric oncology (systematic review)
https://link.springer.com/article/10.1007/s41547-024-00249-xSystematic review: LLLT in children with cancer
https://adc.bmj.com/content/107/2/128PBM as prevention for oral mucositis (systematic review)
https://www.sciencedirect.com/science/article/pii/S0300571225005202LLLT in oral surgery (systematic review)
https://www.sciencedirect.com/science/article/pii/S1572100025001231PBM and tissue healing (RCT systematic review)
https://www.mdpi.com/2077-0383/15/2/613PBM in oral/maxillofacial surgery
https://link.springer.com/article/10.1007/s41547-025-00312-1LLLT and postoperative healing meta-analysis
https://link.springer.com/article/10.1007/s10103-020-03072-5PBM for pain, swelling, and trismus (systematic review)
https://www.joms.org/article/S0278-2391%2823%2900468-8/fulltextPBM mechanisms + growth factors review
https://www.mdpi.com/2304-6732/10/10/1095
📳 Vibration Therapy
Evidence Level: Moderate + Emerging (Condition-Specific)
Vibration-based interventions show promising results, especially in motor function and regulation.
Key Research:
Whole-body vibration in children with cerebral palsy (meta-analysis)
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0282604WBV therapy RCT meta-analysis (CP)
https://academic.oup.com/ptj/advance-article/doi/10.1093/ptj/pzaf052/8111445WBV musculoskeletal outcomes (systematic review)
https://www.mdpi.com/2077-0383/12/21/6759WBV effects on tone and function (meta-analysis)
https://www.scienceopen.com/hosted-document?doi=10.57197/JDR-2023-0056WBV systematic review (mobility + balance)
https://eresearch.qmu.ac.uk/items/5c3f1e98-082e-48a7-8309-1cad21d70270Vibroacoustic therapy in autistic children (pilot study)
https://www.mdpi.com/2227-9032/13/5/465Sensory-based interventions review (includes vibration tools)
https://www.frontiersin.org/journals/pediatrics/articles/10.3389/fped.2025.1720179/pdfAOTA sensory intervention systematic review
https://research.aota.org/ajot/article/76/Supplement_1/7610510189p1Evidence review: sensory-based OT interventions
https://www.epistemonikos.org/en/documents/eb9bbb525f64ad82f485f9fe816edade0f71d80cPediatric feeding review (includes multisensory + vibration approaches)
https://research.aota.org/ajot/article/80/1/8001185010/28487
⚖️ Weighted Materials & Deep Pressure
Evidence Level: Mixed / Individualized Response
Deep pressure is widely used clinically, though research shows variable outcomes.
Key Research:
Weighted blankets RCT in autism
https://europepmc.org/article/MED/25022743Weighted blankets single-subject pediatric study
https://www.mdpi.com/2227-9067/8/1/10Weighted blanket follow-up study (ADHD/ASD)
https://www.tandfonline.com/doi/pdf/10.1080/11038128.2021.1939414Deep pressure (hug machine) pilot study
https://europepmc.org/article/MED/10200837Immediate effects of deep pressure study
https://pmc.ncbi.nlm.nih.gov/articles/PMC5612681/Weighted vest systematic review (not yet evidence-based)
https://www.sciencedirect.com/science/article/pii/S1750946717300387Weighted vest attention study (OT)
https://research.aota.org/ajot/article/55/6/629Weighted vest randomized study (mixed results)
https://link.springer.com/article/10.1007/s10803-010-1104-xCompression garment study
https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2023.1292439Weighted vest single-subject research
https://files.eric.ed.gov/fulltext/ED490780.pdf
🌀 Sensory Integration & Sensory-Based Interventions
Evidence Level: Moderate to Strong (Varies by Approach)
Ayres Sensory Integration® has stronger evidence, while general sensory-based tools show more variability.
Key Research:
Ayres Sensory Integration systematic review
https://research.aota.org/ajot/article/79/3/7903205180ASI systematic review for autism
https://onlinelibrary.wiley.com/doi/epdf/10.1002/aur.2046Sensory integration therapy review (2013–2023)
https://www.mdpi.com/2227-9067/11/10/1222Sensory integration meta-analysis
https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2025.1623149Sensory interventions systematic review (AOTA)
https://research.aota.org/ajot/article/76/Supplement_1/7610510189p1Sensory-based interventions review
https://www.frontiersin.org/journals/pediatrics/articles/10.3389/fped.2025.1720179/pdfOT sensory intervention effectiveness review
https://research.aota.org/ajot/article/74/4_Supplement_1/7411520500p1Sensory-based OT practice overview
https://research.aota.org/ajot/article/79/Supplement%201/7910393020Sensory integration RCT
https://link.springer.com/article/10.1007/s10803-025-06970-1ASI randomized controlled trial (functional outcomes)
https://research.jefferson.edu/labs/researcher/schaaf-laboratory/publications.html
🧠 Reflex Integration / Primitive Reflex Development
Evidence Level: Emerging + Mixed
Primitive reflexes are automatic movement patterns present in infancy that support early development. As the nervous system matures, these reflexes are expected to integrate, allowing for more voluntary, coordinated movement.
In some children, reflexes may remain active beyond typical developmental timelines. Research suggests this can be associated with differences in:
Motor coordination
Balance and posture
Sensory processing
Attention and regulation
Feeding and oral function
What the Research Shows
Current research supports a relationship between retained reflexes and functional challenges, particularly in motor and sensory domains. Some studies also suggest links to attention and learning differences.
There is early but growing research exploring intervention approaches, including movement-based and exercise programs that may help reduce retained reflex patterns and support functional outcomes.
At this time:
Evidence for associations is stronger than evidence for specific reflex integration protocols
Intervention research is promising but still developing
Outcomes are often best when reflex-based work is part of a broader, individualized therapy approach
Key Research
Retained primitive reflexes in autism and implications for intervention
https://www.frontiersin.org/journals/neurology/articles/10.3389/fneur.2022.922322/fullPrimitive reflexes as biomarkers for developmental differences
https://onlinelibrary.wiley.com/doi/pdf/10.1111/jpc.70053Persistence of primitive reflexes in developmental disorders
https://link.springer.com/content/pdf/10.1007/s40474-021-00232-2.pdfPrimitive reflexes, learning, and motor function (systematic review)
https://www.unboundmedicine.com/medline/citation/35830652Primitive reflexes and ADHD
https://link.springer.com/article/10.1007/BF03379591Reflex activity and motor skill performance in preschool children
https://www.mdpi.com/2076-3425/11/8/967Reflex activity and sensory processing differences
https://www.mdpi.com/1660-4601/17/21/8210ATNR influence on gait and symmetry
https://www.mdpi.com/1660-4601/17/13/4759Primitive reflexes and gait development
https://www.mdpi.com/1660-4601/19/7/4070Exercise-based intervention and reflex integration outcomes
https://www.mdpi.com/2227-9067/12/8/987
How We Use This in Therapy
At B.well tots, reflex-based work is:
Integrated into functional therapy, not used in isolation
Movement-based and play-based, aligned with development
Responsive to your child’s cues and tolerance
We do not follow rigid protocols. Instead, we focus on:
Supporting nervous system organization
Improving functional movement and coordination
Enhancing regulation and participation in daily activities
Our Approach to Evidence
We believe in being transparent and thoughtful about emerging areas of care.
For reflex integration, this means:
Using current research to guide—not dictate—practice
Combining evidence with clinical expertise
Prioritizing what is meaningful and effective for your child
What This Means for Your Child
Reflex-based strategies may be used to support:
Coordination and motor planning
Postural control
Regulation and attention
Feeding and oral-motor function
These strategies are always:
✔ Individualized
✔ Optional
✔ Part of a comprehensive plan of care
The Science Behind ICR Technology
The ICR (Ion Cyclotron Resonance) Mat is grounded in emerging research exploring how low-frequency electromagnetic and capacitive interactions influence the nervous system and cellular signaling.
How It Works (Simplified)
At a biological level, the body relies on electrical signaling between cells, especially within the nervous system. These signals depend on the movement of ions like sodium (Na⁺) and potassium (K⁺) across cell membranes.
Research shows that:
External electromagnetic or capacitive inputs can influence ion movement and membrane potential
This can impact how signals are transmitted along nerves
And ultimately affect movement, coordination, and regulation of the body
This process is often described as neuromodulation—supporting the body’s ability to regulate its own signaling systems.
What Research Demonstrates
Recent studies on similar technologies have explored how low-frequency electromagnetic or capacitive devices may:
Modulate neuronal activity by influencing ion channels and membrane potentials
Improve motor control, coordination, and postural stability in neurological populations
Influence inflammatory and cellular signaling pathways, including cytokine activity
Support nervous system regulation and functional improvements in developmental and neurological conditions
Importantly, these approaches are:
Non-invasive
Drug-free
Designed to work alongside the body’s existing systems
Why This Matters for Development
Early development is a period of rapid neurological change. During this time:
The brain and body rely heavily on sensory input and movement
Neural pathways are shaped through repetition, positioning, and environmental interaction
Emerging evidence suggests that supporting the electrical and sensory environment of the body may:
Enhance communication between systems
Improve regulation and coordination
Complement movement-based and therapeutic approaches
How the ICR Mat Fits In
The ICR Mat is designed to provide consistent, low-level input to the body’s sensory and neurological systems during rest and play.
Rather than forcing change, it supports:
Natural movement exploration
Sensory integration
Whole-body regulation
This aligns with a growing body of research showing that environment + input + repetition = meaningful developmental change.
Our Clinical Perspective
At B.Well Tots, we view tools like the ICR Mat as supportive—not standalone solutions.
They are most effective when combined with:
Movement-based therapy
Positioning strategies
Feeding and oral function support
Whole-child developmental care
Because real progress comes from supporting the nervous system as a whole—not just one piece of it.
Our Philosophy on Evidence
Not all therapies fit neatly into “proven” or “not proven.”
At B.well tots, we practice:
Evidence-informed care (not trend-based)
Clinical reasoning + ongoing education
Child-led, response-driven treatment
Some interventions are:
✔ Strongly supported
✔ Emerging with promising evidence
✔ Best used as part of a comprehensive, individualized plan
Remember, it takes on average SEVENTEEN YEARS for research to be implemented into practice.
Questions? We’re Here.
We welcome questions about:
Why a modality is being used
What the research says
Alternatives or modifications
👉 Have more questions? Let us know!
👉 Or ask your provider anytime during your session!
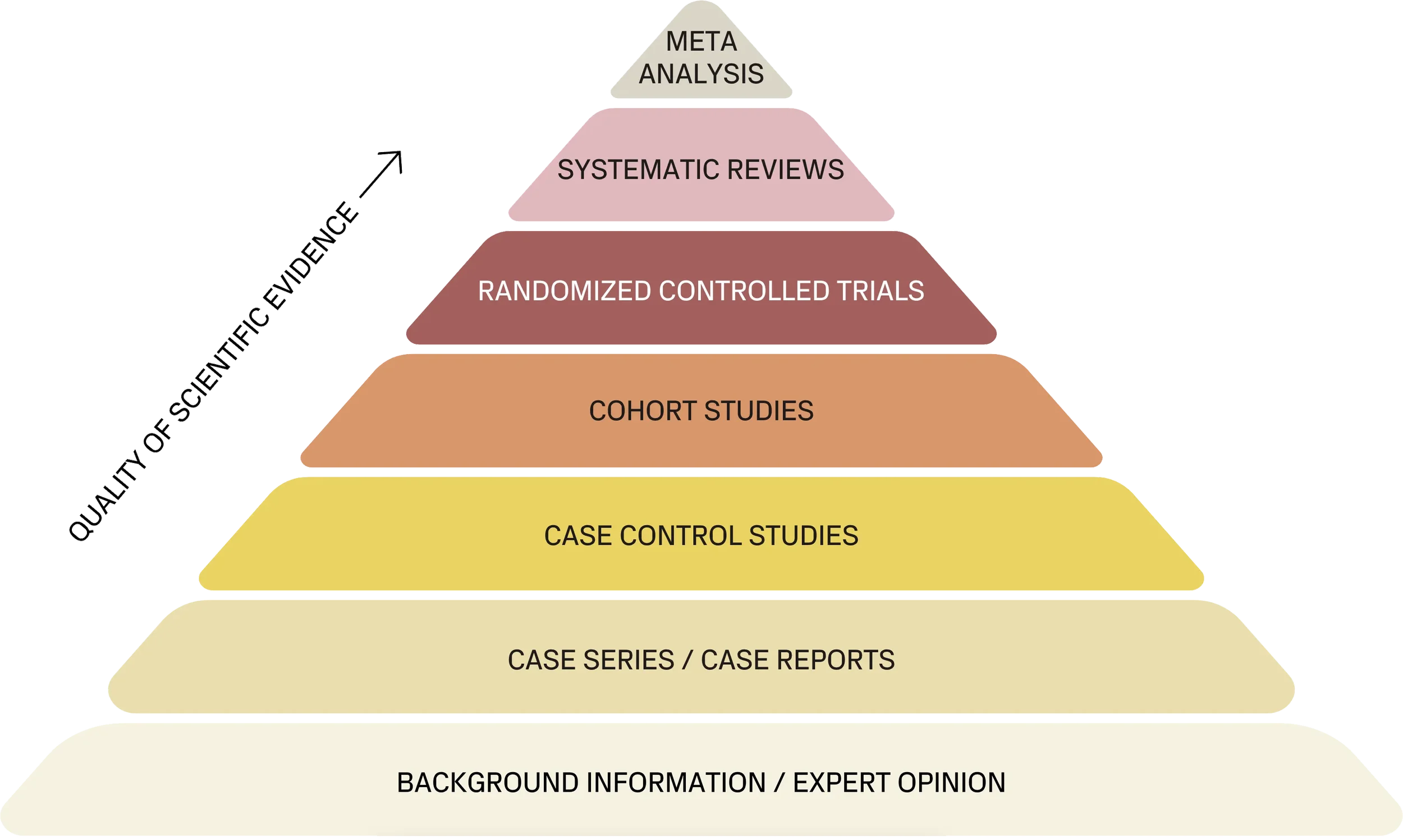
The information above reflects current published research and clinical findings. While evidence is strong in many medical applications, pediatric research is still evolving. All treatment decisions should be made in collaboration with qualified healthcare professionals and tailored to each individual child.
